Ophthalmology | Last Updated: February 20, 2023
Cornea Transplantation: Everything You Need To Know
A cornea transplant, also known as keratoplasty, is a surgical procedure to replace a damaged or diseased cornea with a healthy one from a donor. The purpose of this procedure is to restore vision and improve the overall health of the eye.
This post aims to provide a comprehensive guide for those seeking information about cornea transplant. The post will cover the different types of cornea transplant procedures, the indications for surgery, preoperative evaluation, the surgical process, postoperative care, and potential risks and complications associated with cornea transplant. The goal is to empower patients with knowledge and understanding of the procedure to make informed decisions about their eye health.
What is a Cornea Transplant?
A cornea transplant is a surgical procedure where a damaged or diseased cornea is replaced with a healthy one from a donor. The cornea is the clear outer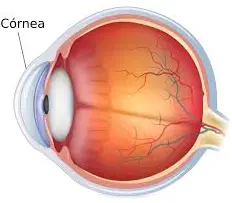 layer of the eye that helps focus light and provides protection to the iris and lens.
layer of the eye that helps focus light and provides protection to the iris and lens.
A cornea transplant is necessary when the patient's cornea becomes cloudy or misshapen, causing vision loss or other eye problems. Some common causes for a cornea transplant include:
- Keratoconus, a condition where the cornea bulges outward and becomes cone-shaped, distorting vision
- Scarring from infections, injuries, or other eye conditions
- Fuch's Dystrophy, a genetic condition that causes the cornea to become clouded
- Previous LASIK or other corneal surgery that has failed
Types of Cornea Transplant
There are two main types of cornea transplants: Full-thickness Transplant and Partial-thickness Transplant.
-
Full-thickness Transplant,
also known as penetrating keratoplasty, involves removing the entire damaged cornea and replacing it with a donor cornea.
-
Partial-thickness Transplant,
also known as lamellar keratoplasty, involves removing only the damaged outer layer of the cornea and replacing it with a thin layer of healthy donor tissue.
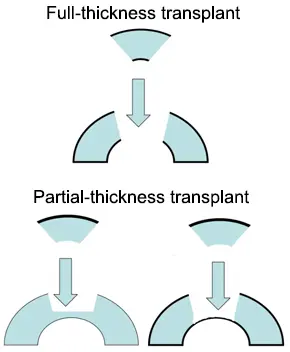
The type of transplant performed will depend on the extent of the patient's corneal damage, location of the damage to the cornea and the surgeon's recommendation.
-
Penetrating Keratoplasty (PKP):
This is the traditional method of cornea transplant, in which a circular button-shaped section of the cornea is removed and replaced with a healthy donor cornea that is secured with sutures. PKP is typically used for cases of severe corneal scarring or thinning, or when multiple layers of the cornea are affected. However, the procedure is associated with a higher risk of complications and a longer recovery time compared to more modern techniques.
-
Endothelial Keratoplasty (EK):
This type of cornea transplant is used to treat diseases affecting the innermost layer of the cornea, such as Fuchs' dystrophy and some cases of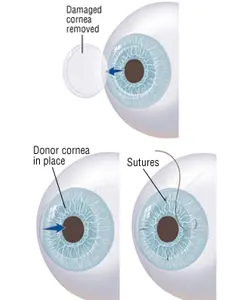 corneal swelling. In EK, only the damaged endothelial layer of the cornea is replaced with a healthy donor graft. There are two types of EK procedures:
corneal swelling. In EK, only the damaged endothelial layer of the cornea is replaced with a healthy donor graft. There are two types of EK procedures:
-
Descemet's Stripping Endothelial Keratoplasty (DSEK):
In this procedure, a thin layer of the patient's cornea is removed and replaced with a similar-sized piece of healthy donor tissue that contains endothelial cells. The donor tissue is held in place with an air bubble until it heals and adheres to the patient's cornea. -
Descemet's Membrane Endothelial Keratoplasty (DMEK):
DMEK is a newer and more technically demanding procedure than DSEK. In DMEK, only the damaged Descemet's membrane and endothelial cells are replaced with an ultra-thin layer of donor tissue. This results in a quicker recovery time, better visual outcomes, and fewer complications compared to PKP and DSEK.
-
-
Deep Anterior Lamellar Keratoplasty (DALK):
This type of cornea transplant is used to treat corneal diseases that affect the outer layers of the cornea, such as keratoconus and corneal scarring. In DALK, the outer layers of the patient's cornea are removed and replaced with healthy donor tissue, while the innermost layer (Descemet's membrane and endothelium) is left intact. This results in a lower risk of rejection and better visual outcomes compared to PKP.
-
Artificial Cornea Transplant:
In some cases, a cornea transplant may not be an option due to various factors such as rejection of donor tissue or a shortage of corneal grafts. In these cases, an artificial cornea, also known as a keratoprosthesis, may be used.
It is important to note that the type of cornea transplant procedure used will depend on the individual patient's condition and the preferences of the surgeon performing the procedure. Your surgeon will be able to determine the most appropriate type of cornea transplant for you.
Benefits of a Cornea Transplant
-
Improved Vision:
One of the primary benefits of a cornea transplant is improved vision. The procedure replaces a damaged or diseased cornea with a healthy one, allowing for clearer and sharper vision. The success rate of cornea transplants is high, with many patients reporting significant improvements in their vision after the procedure.
-
Reduction of Pain and Discomfort:
Another advantage of a cornea transplant is the reduction of pain and discomfort. A damaged or diseased cornea can cause significant discomfort, including pain, sensitivity to light, and redness. A cornea transplant can help to alleviate these symptoms and provide relief to patients who have been suffering from them.
-
Better Quality of Life:
A cornea transplant can also lead to a better quality of life for patients. Improved vision allows patients to perform daily tasks more easily, engage in activities they enjoy, and generally feel more confident and independent. This can result in a significant improvement in overall well-being and a more positive outlook on life.
Preparing for a Cornea Transplant
-
Consultation with an Ophthalmologist:
Before undergoing a cornea transplant, it is important to have a consultation with an ophthalmologist. The ophthalmologist will evaluate the patient's current condition and determine if a cornea transplant is the best option. During the consultation, the ophthalmologist will also discuss the procedure, including the type of transplant that will be performed, and answer any questions the patient may have.
-
Evaluating Eligibility:
To be eligible for a cornea transplant, patients must meet certain criteria. These criteria include good general health, stable eye condition, and the absence of certain medical conditions that may interfere with the healing process. The ophthalmologist will evaluate the patient's overall health and perform a comprehensive eye exam to determine eligibility for the procedure.
-
Understanding the Risks and Side Effects:
As with any surgical procedure, a cornea transplant carries certain risks and side effects. The ophthalmologist will explain these risks and side effects to the patient, including the risk of rejection, infection, and vision loss. It is important for patients to have a full understanding of these risks and side effects before deciding to undergo a cornea transplant.
The Cornea Transplant Procedure
-
Surgical Preparation:
Before a cornea transplant, the patient will have an initial consultation with their ophthalmologist to determine if they are a suitable candidate for the procedure. During this time, the patient will undergo a thorough eye exam to evaluate the extent of their vision problems and to determine if a cornea transplant is the best course of action. The patient will also be given a detailed explanation of the procedure, the expected outcomes, and the risks involved.
-
The Procedure itself:
The cornea transplant procedure typically takes between 1-2 hours and is performed under local anesthesia. During the procedure, the surgeon will carefully remove the damaged or diseased cornea and replace it with a healthy cornea from a donor. The donor cornea is carefully matched to the recipient's eye to ensure a good fit and optimal vision. The surgical site is then carefully closed, and the eye is covered with a patch or protective shield to prevent infection and promote healing.
-
Post-Operative Care and Recovery:
After the procedure, the patient will need to follow a strict regimen of post-operative care to promote healing and reduce the risk of complications. This typically includes the use of eye drops, wearing a protective shield, and avoiding activities that could put pressure on the eye. The patient will also need to attend regular follow-up appointments with their ophthalmologist to monitor the healing process and to ensure that the transplant is successful. Most patients will notice improved vision within a few days to weeks after the procedure, and a full recovery can take several months.
Potential Complications and Risks
As with any surgical procedure, there are potential complications and risks associated with cornea transplant. Although most people experience a successful outcome, it's important to be aware of the potential complications before making the decision to undergo the procedure.
-
Rejection:
One of the most serious risks associated with cornea transplant is the possibility of rejection. This occurs when the body's immune system recognizes the donor cornea as foreign and attacks it. Signs of rejection may include redness, pain, sensitivity to light, and decreased vision. It's important to seek medical attention right away if you experience any of these symptoms.
-
Infection:
Infection is another potential complication of cornea transplant. The risk of infection can be reduced by following your doctor's post-operative instructions carefully and taking any prescribed medications as directed.
-
High eye pressure:
Cornea transplant can cause elevated eye pressure, which can lead to glaucoma. Your doctor will monitor your eye pressure after surgery and prescribe medications if necessary to prevent this complication.
-
Astigmatism:
Cornea transplant can cause astigmatism, which is an irregular curvature of the cornea that can affect vision. In some cases, eyeglasses or contact lenses can correct this problem. In more severe cases, a second cornea transplant may be necessary.
-
Cataracts:
Cornea transplant can increase the risk of developing cataracts, which are a clouding of the lens of the eye. If cataracts develop, they can be treated with surgery.
-
Other potential complications:
Other potential complications of cornea transplant include bleeding, swelling, and pain. These complications are rare, but it's important to be aware of them.
Conclusion
In conclusion, a cornea transplant is a surgical procedure that can help restore vision and improve the quality of life for individuals suffering from various corneal conditions. It is a safe and effective procedure that has been performed for many years with a high success rate.
However, it is important to prepare for the procedure and understand the potential risks and complications. It is also important to consider the cost of the procedure and to find a skilled and experienced surgeon. In some cases, an artificial cornea may be an option for those who are not candidates for traditional cornea transplants. If you or a loved one is considering a cornea transplant, it is important to consult with a qualified healthcare professional to determine if it is the right option for you. With proper preparation and care, a cornea transplant can greatly improve vision and quality of life.
Frequently Asked Questions (FAQs) about Cornea Transplant
What is the success rate of cornea transplant surgery?
The success rate of cornea transplant surgery varies depending on the type of procedure and the underlying condition. In general, the success rate of PK is about 90%, while the success rate of DALK is about 80%. The success rate of DMEK is about 95%.
How long does it take to recover from cornea transplant surgery?
The recovery time after cornea transplant surgery varies depending on the type of procedure and the individual's overall health. In general, it takes about 6-12 months for the vision to stabilize and for the eye to fully heal.
What is the cost of cornea transplant surgery in India?
The cost of cornea transplant surgery varies depending on the type of procedure and the location. In the India, the average cost of cornea transplant surgery ranges from $1800 to $2000.
How long does a cornea transplant last?
The lifespan of a cornea transplant varies depending on the individual and the underlying condition. In general, a cornea transplant can last anywhere from 5 to 20 years or more.
Is it possible to reject a cornea transplant?
Yes, it is possible to reject a cornea transplant. The risk of rejection can be reduced by taking medications as prescribed and following the doctor's instructions for post-operative care.






